Sciatica is a huge problem. It can completely disrupt your life. It can limit you from all the activities you love to do because it can be painful to sit, stand, walk, sleep, or all of the above. It can be scary because it may seem like nothing you do is helping, or you may not be sure what to do for fear of making things even worse. As physical therapists, we understand these concerns and we are here to help you and reassure you. The purpose of this article is to bring you hope and information that can help allay some fears and concerns, and ultimately guide you back to being in control of your Sciatica.
What is Sciatica?
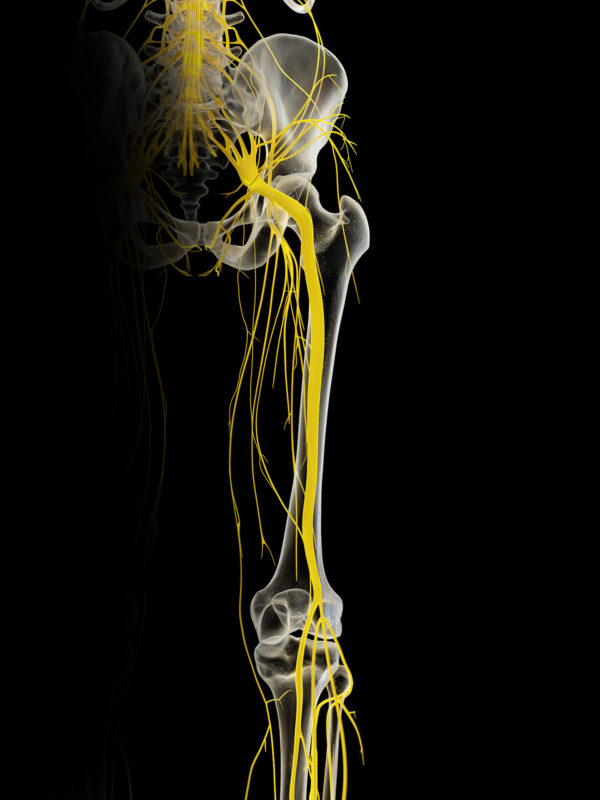
Sciatica is a non-specific umbrella term to describe symptoms of discomfort down the leg. Pain, burning, numbness, tingling, pins and needles are some of the more common symptoms we hear. Sometimes, it can even be difficult to describe what you feel. We call it “Sciatica” because your sciatic nerve runs down the back of your thigh, however, the problem is most likely in your lower back region. You may not even have back pain and still be experiencing sciatica. Nerve roots from your lower spine come together to form the sciatic nerve. It is likely that one or more of those nerve roots are irritated but the symptoms are present in the buttock or thigh.
Is sciatica dangerous?
In the overwhelming majority of cases sciatica is not a dangerous situation. This condition has a favorable outcome most of the time. More serious symptoms are when leg muscles become increasingly weak (foot drop, knee buckling), you have bowel and bladder changes (urinary retention, incontinence), or your symptoms are constant and no body position or movement changes your pain. These are what we call red flags and are rare situations. They occur in less than one percent of all people with sciatica.
What are the causes of sciatica?
DISC HERNIATION
In many cases the discs of your spine are the cause of sciatica. The discs in our backs are made of an incredibly strong outer layer called the annulus fibrosis. They also have a more gelatinous inner layer called the nucleus pulposus. This inner layer can sometimes push through the outer layer and can put a mechanical compression on the nerve as well act as a chemical irritant to the nerve roots. When this happens it can manifest in pain and discomfort into the buttocks and legs.
There are several classifications of disc herniation depending on how much of the inner layer has moved from its original position. It had been previously thought that these herniations are permanent, but research tells us that discs can heal on their own without surgery.
DISC DEGENERATION
This is a little different than a herniation because it usually happens later in life. Disc degeneration sounds like a scary term, and sometimes people get hung up on this diagnosis, but it is important to understand that ALL of our discs degenerate to some degree. It is just a fact of life as we age. It’s similar to skin wrinkling over time, our tissues simply become less elastic. While still strong, the collagen in the outer portion in the disc starts to thin and the inner portion tends to leak out and cause irritation on the nerves. Now, there is still a lot we do not understand about degenerative disc disease and how it correlates to pain and sciatica. There is overwhelming evidence that shows many people without pain have similar MRI fings to those that have pain. This is good news because it provides hope to those who have been told they have degenerative disc disease. Degenerative disc disease does not mean you have a bad back, it most likely means you have a normal back that has the potential to get stronger and become less painful.
Should you get an MRI?
An MRI is usually only indicated for surgical planning. It will not change how your physical therapist manages your rehab. Oftentimes, an MRI doesn’t always correlate to your symptoms anyway, and on top of that an MRI can show things that are not even causing your symptoms. We know this because there have been studies where symptomatic patients and non symptomatic patients have the same findings. An MRI can also create unnecessary fear. As I said before, the spine is incredibly strong and capable of withstanding compression, shear, and tension forces even when an MRI shows findings. The physical therapist’s job is to help empower you to return to function and not to change what is on the MRI.
How about Surgery?
I am not a surgeon, therefore, I am not going to give surgical advice. But I will say this, physical therapy and rehab are almost always the preferred option, especially to start. There is less risk and less cost associated with conservative rehab. The long term outcomes are roughly the same when managed conservatively and with surgery.
-Remember, our spines are strong, our discs are strong and our bodies are adaptable and resilient.
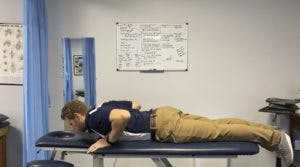
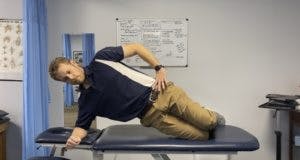
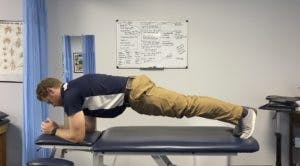
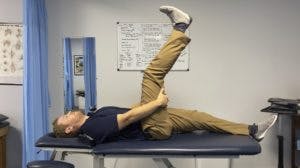
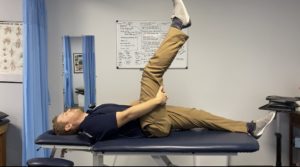
Sciatica Treatment and Exercises
Unfortunately, there isn’t a perfect exercise or combination of exercises for sciatica because every case is different. A PT’s exam will determine the best course of treatment for your particular sciatica. It will depend on many variables such as how recent your pain started, what are the causes of your symptoms, what makes them better, nature of pain, and many other variables. What works for you may not work for another person. I will list some basic exercises commonly prescribed for sciatica treatment, but our exam will determine the best approach and this should not be taken as a cure all. Of course, every person is different. We will always treat the individual and not the diagnosis. To get started for sciatica treatment in Goose Creek, Charleston, and Mount Pleasant, give us a call at (843) 793-4466. Or CLICK HERE for our contact info.